CLINICAL STUDY - COMPANION B-15 Sub-study Primary Endpoint and Additional Tertiary Endpoints Exercise performance––the co-primary endpoint, which consists of Peak VO2 and Six-Minute Walk, is designed to demonstrate improvement in exercise performance with CRT (CONTAK TR and CONTAK CD pooled data) compared to OPT at six months post-baseline. Additional tertiary endpoints included Quality of Life as measured by the Minnesota Living with Heart Failure Questionnaire® and NYHA Class.
B-16 CLINICAL STUDY - COMPANION Table B-5. Patient population characteristics for COMPANION (OPT and CRT-D) OPT (N = 308) CRT-D (N = 595) P-value Mean ± SD 66.7 ± 10.7 65.6 ± 11.2 0.14 Female 97 (31.4) 194 (32.6) 0.73 Male 211 (68.5) 401 (67.3) 0.73 Class III 253 (82.1) 512 (86.1) 0.12 Class IV 55 (17.8) 83 (13.9) 0.12 Ischemic 58.7 54.6 0.13 Non-ischemic 41.3 45.4 0.13 LVEF (%) Mean ± SD 22.8 ± 7.2 22.5 ± 6.8 0.
CLINICAL STUDY - COMPANION B-17 account for patients that had a hospitalization or death event that contributed to the primary endpoint or secondary endpoint of all-cause mortality. Table B-6. Patient follow-up disposition 12 months post-randomization CRT-D # of # of Withdrawn Deceased Patients Patients OPT (N = 595) # Reached end of study (Nov. 30, 2002) # of Active Patients at end of time interval # of # of Withdrawn Deceased Patients Patients (N = 308)# Reached end of study (Nov.
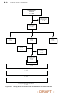
B-18 CLINICAL STUDY - COMPANION COMPANION Enrolled n = 1638 Fall out prior to Randomization n = 118 Randomized n = 1520 Randomized to OPT n = 308 Randomized to CRT-D n = 595 Randomized to CRT-P n = 617 CRT-D Implant Intents n=7 CRT-D Implant Attempts n = 47 Implanted CRT-D Devices n = 541 System Safety Endpoint n = 541 All-cause mortality endpoint through 12/1/02 for OPT and CRT-D n = 903 All adverse events through 11/26/03 for OPT and CRT-D n = 903 All-cause mortality or first hospitalization
CLINICAL STUDY - COMPANION B-19 Event Contributing to Primary Endpoint and Secondary Endpoint of All-cause Mortality A total of 903 COMPANION patients in the CRT-D (595) and OPT (308) groups were eligible for the primary endpoint. Figure B-2 on page B-19 provides patient randomization and status for the primary endpoint and Figure B-3 on page B-19 provides patient randomization and status for the secondary mortality endpoint.
B-20 CLINICAL STUDY - COMPANION DATA ANALYSIS AND RESULTS FOR PRIMARY ENDPOINT AND SECONDARY ALL-CAUSE MORTALITY ENDPOINT Sequential Monitoring The COMPANION DSMB met approximately every six months to review the trial’s progress and to review the safety and effectiveness data collected. An “O’Brien-Fleming” type boundary as implemented by Lan and DeMets was used in monitoring the trial.
CLINICAL STUDY - COMPANION B-21 All-cause Mortality or First Hospitalization 100 CRT-D vs. OPT: p = 0.010 80 % of Patients Event-Free OPT CRT-D Number of Events OPT: 216 CRT-D: 390 60 40 20 HR = 0.80. 95% CI (0.68, 0.95) 0 0 120 240 360 480 600 720 840 960 16 25 6 8 1 0 1080 Days from Randomization Number of Patients at Risk Figure B-4.
B-22 CLINICAL STUDY - COMPANION depicted in Figure B-5 on page B-22. These numbers correspond to an annual mortality rate of 19% in the OPT arm and 12% in the CRT-D arm, with a hazard ratio of 0.64, 95% CI (0.48, 0.86). These results demonstrated that CRT-D was associated with a 36% reduction in the risk of all-cause mortality when compared to OPT alone. All-cause Mortality CRT-D vs. OPT: p = 0.003 100 OPT CRT-D Number of Events OPT: 77 CRT-D: 105 % of Patients Event-Free 90 80 70 60 HR = 0.64.
CLINICAL STUDY - COMPANION Table B-8. B-23 Mortality endpoint risk reduction point estimates (continued) % Failure Absolute Risk Reduction Relative Risk Reduction OPT CRT-D 12 months 18.9% (14.1%, 23.5%) 12.1% (9.3%, 14.8%) 6.8% 36.0% 18 months 28.4% (22.3%, 34.1%) 18.0% (14.4%, 21.5%) 10.4% 36.6% Results for Secondary Cardiac Morbidity Endpoint During a hospitalization more than one of the pre-specified cardiac morbid events could occur.
B-24 CLINICAL STUDY - COMPANION Frequency (per Patient) Frequency (per Patient Year) Duration 36% reduction p < 0.0001 52% reduction p < 0.0001 41% reduction p < 0.0001 60 1.2 8 1.08 50 7.6 40 35% 30 20 0.8 0.6 0.52 0.4 10 0.2 0 0.0 OPT (n = 308) Figure B-6. Duration (Days/Patient-Year) 1.0 Event Rate (Events/Patient-Year) Proportion of Patients with ≥ 1 Event (%) 55% 6 4.
CLINICAL STUDY - COMPANION B-25 For a given cardiac hospitalization, patients may have events in more than one category, and if there are multiple occurrences in a single category, then only the first occurrence was counted. ADDITIONAL STUDY DATA Implant Disposition Table B-9 on page B-25 identifies the number of initial and subsequent implant procedures attempted in patients randomized to CRT-D and the rate of success for each additional implant procedure.
B-26 CLINICAL STUDY - COMPANION • Use of intravenous inotropes and/or vasoactive drugs for a duration > 4 hours (inpatient or outpatient) NOTE: Hospitalizations associated with a device implant attempt or re-attempt are excluded.
CLINICAL STUDY - COMPANION B-27 All-cause Mortality or First Heart Failure Hospitalization CRT-D vs. OPT: p < 0.001 100 OPT CRT-D Number of Events OPT: 145 CRT-D: 212 % of Patients Event-Free 80 60 40 20 HR = 0.60. 95% CI (0.49, 0.75) 0 0 120 240 360 480 600 720 840 960 28 71 11 27 2 5 1080 Days from Randomization Number of Patients at Risk Figure B-8.
B-28 CLINICAL STUDY - COMPANION are normalized per patient-year of follow-up. An additional comparison of hospitalization days for heart failure hospitalizations is shown in Figure B-11 on page B-29. NOTE: CRT-D was associated with a reduction in all-cause mortality and therefore there is a competing risk for hospitalizations. This data should be interpreted with caution. 2.5 2.01 Hospitalizations (In-patient) per Patient-Year of Follow-up 2.0 1.62 1.5 Initial Implant 0.07 Initial Implant 0.83 1.
CLINICAL STUDY - COMPANION 5.9 6 Heart Failure Hospitalization Days per Patient-Year of Follow-up B-29 5 4 3.8 3 2 1 0 OPT (n = 308) Figure B-11. CRT-D (n = 595) Heart failure hospitalization days per patient year DATA ANALYSIS AND RESULTS - CRT-D SYSTEM SAFETY The system-related complication-free rate analysis was not a predefined endpoint in the protocol. The intent of this analysis is to provide reasonable assurance of safety of the CONTAK CD system in this patient population.
B-30 CLINICAL STUDY - COMPANION DATA ANALYSIS AND RESULTS - COMPANION SUB-STUDY The Exercise Performance Sub-study consisted of the following components. CRT Effectiveness Primary Co-primary endpoint consisting of Peak VO2 derived from a symptom-limited exercise test and Six-Minute Walk, with CRT results pooled from the CONTAK TR and CONTAK CD arms. Effectiveness was determined by assessing both Peak VO2 and Six-Minute Walk distance improvements with CRT compared to OPT.
CLINICAL STUDY - COMPANION B-31 Patient Accountability (Figure B-12 on page B-31) Randomized 448 Intent/Attempt 37 Met Exclusion Criteria 6 CRT Baseline Visit 318 OPT Baseline Visit 87 11 Patient related 6 28 Patient related 24 10 Crossover 5 21 Mode Change 3 10 Withdrawn 10 2 Withdrawn 2 4 Death 4 16 Death 16 6 Other 5 20 Other 12 Peak VO2 Assessable for effectiveness 46 Figure B-12.
B-32 CLINICAL STUDY - COMPANION Table B-10. Patient population characteristics (continued) CRT (N = 318) OPT (N = 87) P-valuea Ischemic 141 (44.3) 42 (48.3) 0.51 Non-ischemic 177 (55.7) 45 (51.7) Mean ± SD 22.5 ± 6.9 22.2 ± 8.0 5.0–35.0 5.0–35.0 Mean ± SD 73.1 ± 12.8 73.5 ± 11.5 Range 46.0–122.0 54.0–103.0 Mean ± SD 159.2 ± 25.0 155.7 ± 25.8 Range 120.0–276.0 120.0–224.0 LBBB 230 (72.3) 62 (71.3) Nonspecific 54 (17.0) 18 (20.7) RBBB 34 (10.7) 7 (8.0) Mean ± SD 12.
CLINICAL STUDY - COMPANION ∆ = 0.8 p = 0.026 B-33 ∆ = 0.6 p = 0.074 (Critical boundary = 0.10) ∆ Peak VO2 (ml/kg/min) 2.0 1.5 CRT OPT 1.0 0.5 0.0 Mean ± SE 3 6 Time (months) Figure B-13. Table B-11. Maximal Oxygen Consumption Results Maximal Oxygen Consumption Results Peak VO2 (ml/kg/min) CRT P-valuea OPT N Mean ± S.E. N Mean ± S.E. Change at 3 months 247 1.1 ± 0.2 52 0.3 ± 0.4 0.026 Change at 6 months 230 1.2 ± 0.2 46 0.6 ± 0.4 0.074 a.
B-34 CLINICAL STUDY - COMPANION ∆ = 24 p = 0.016 ∆ = 24 p = 0.017 (Critical boundary = 0.05) ∆ Six Minute Walk Distance (m) 50 40 30 CRT OPT 20 10 0 Mean ± SE 3 6 Time (months) Figure B-14. Table B-12. Change in six-minute walk Change in six-minute walk CRT Six-Minute Walk (m) P-valuea OPT N Mean ± S.E. N Mean ± S.E. Change at 3 months 274 37 ± 5 63 13 ± 10 0.016 Change at 6 months 260 41 ± 5 57 17 ± 10 0.017 a.
CLINICAL STUDY - COMPANION CRT OPT CRT B-35 OPT 100 80 NYHA Class (%) Improve 2 Classes Improve 1 Class No Change 60 Worsen 1 Class 40 20 0 3 6 Time (months) Figure B-15. Table B-13. Change in NYHA Change in NYHA NYHA Classification 3 months 6 months Change Improve 2 Classes CRT P-valuea OPT N Patients N Patients 294 22 (7.5%) 69 3 (4.4%) Improve 1 Class 142 (48.3%) 13 (18.8%) No Change 122 (41.5%) 48 (69.6%) Worsen 1 Class 8 (2.7%) 5 (7.
B-36 CLINICAL STUDY - COMPANION ∆ = 17 ∆ = 13 30 ∆ Quality of Life Score (points) 25 20 15 CRT OPT 10 5 0 Mean ± SE 3 6 Time (months) Figure B-16. Table B-14. Quality of Life score Quality of Life score Quality of Life (points) CRT P-valuea OPT N Mean ± S.E. (95% CI) N Mean ± S.E. (95% CI) Change at 3 months 289 23 ± 1 (20.1, 25.7) 72 6 ± 3 (0.6, 11.3) < 0.001 Change at 6 months 279 23 ± 1 (19.7, 25.4) 66 10 ± 3 (4.2, 15.2) < 0.001 a.
CLINICAL STUDY - COMPANION Table B-15. B-37 Changes in six-minute walk, QOL, and NYHA (continued) CRT-D P-valuea OPT 377 45 ± 98 141 2 ± 92 N Mean ± SD N Mean ± SD Change at 3 months 514 -24 ± 28 243 -8 ± 21 < 0.0001 Change at 6 months 479 -23 ± 28 207 -12 ± 23 < 0.0001 N % Improved N % Improved Change at 3 months 543 55 242 24 < 0.0001 Change at 6 months 498 57 199 38 < 0.0001 Change at 6 months QOL NYHA < 0.0001 a.
B-38 CLINICAL STUDY - COMPANION - DRAFT -
C-1 CLINICAL STUDY - DECREASE HF APPENDIX C SUMMARY The DECREASE-HF study was designed to determine if LV-CRT and LV Offset are safe and effective as compared to the control treatment (BiV-CRT) in patients with heart failure and an indication for an implantable cardioverter defibrillator (ICD). The primary effectiveness endpoint was a composite of peak VO2 and left ventricular end systolic diameter (LVESD).
C-2 CLINICAL STUDY - DECREASE HF FOLLOW-UP SCHEDULE The follow-up schedule for the DECREASE HF study is detailed below (Table C-1 on page C-2). Table C-1. DECREASE HF follow-up schedule Follow-up period Follow-up schedule Pre-implant Initial assessment of patient eligibility; taking of patient history. Administration of baseline Quality of Life (QOL) questionnaire. Implant Implant of investigational devices and acute device testing.
CLINICAL STUDY - DECREASE HF C-3 • Willing and capable of undergoing a device implant and participating in all testing associated with this clinical investigation • Have a life expectancy of more than 180 days, per physician discretion • Age 18 or above, or of legal age to give informed consent specific to state and national law Patients were excluded from the investigation if they met any one of the following exclusion criteria: • Right bundle branch block morphology (per World Health Organization
C-4 CLINICAL STUDY - DECREASE HF • Were enrolled in any concurrent study, without Guidant written approval, that may confound the results of this study DEMOGRAPHIC DATA Patient enrollment (Figure C-1 on page C-4) and baseline characteristics (Table C-2 on page C-4) are detailed below. Enrolled 360 Intent 2 Attempt 16 Implant 342 Death 1 Death 3 Withdrawal 1 Incomplete Baseline Testing 13 Received Randomization Assignment 325 Expert Ease BiV Suggestion 19 Randomized 306 LV-CRT 101 Figure C-1.
CLINICAL STUDY - DECREASE HF Table C-2. C-5 DECREASE-HF study patient characteristics (continued) Measurement Characteristic BiV-CRT (N=101) 101 104 100 Mean ± SD 22.6 ± 6.6 22.4 ± 6.7 23.2 ± 7.1 Range 8.0 - 35.0 9.0 - 35.0 5.0 - 35.
C-6 CLINICAL STUDY - DECREASE HF STUDY RESULTS Therapy Effectiveness Primary Endpoint Composite Score––Effectiveness of LV Offset was measured using a Composite Score that combines six-month changes in Peak VO2 and LVESD (Figure C-2 on page C-6, Table C-3 on page C-7).
CLINICAL STUDY - DECREASE HF Table C-3. C-7 Composite score equivalence to BiV-CRT at six months Statistic LV Offset BiV-CRT Na Estimate ± SE Na Estimate ± SE 3-Month Composite Score 71 12.4 ± 1.5 70 16.0 ± 1.5 6-Month Composite Score 70 12.8 ± 1.7 76 16.4 ± 1.7 Difference at 6 Months (BiV-CRT - LV Offset) Confidence Interval Upper Bound 3.6 ± 2.4 8.2 a. N refers to the number of patients with paired data.
C-8 CLINICAL STUDY - DECREASE HF All patients with data at a minimum of one visit, N=189 Peak VO2 (ml/kg/min) 15 14 13 12 Baseline 3-Month LV Offset Figure C-3. Table C-4. 6-Month BiV-CRT Improvement in Peak V02 at Six Months Improvement in Peak VO2 at six months Statistic LV Offset Na Baseline BiV-CRT Estimate ± SE Na Estimate ± SE 89 12.7 ± 0.2 88 12.7 ± 0.2 3 Months 72 14.2 ± 0.3 71 14.5 ± 0.3 6 Months 71 14.3 ± 0.3 76 14.2 ± 0.
CLINICAL STUDY - DECREASE HF C-9 All patients with data at a minimum of one visit, N=205 46 48 LVESD (mm) 50 52 54 56 58 Baseline 3-Month LV Offset Figure C-4. Table C-5. 6-Month BiV-CRT Improvement in LVESD at Six Months Improvement in LVESD at six months Statistic LV Offset Na Baseline BiV-CRT Estimate ± SE Na Estimate ± SE 104 55.7 ± 0.5 100 55.7 ± 0.5 3 Months 97 50.5 ± 0.9 97 48.9 ± 0.9 6 Months 92 50.3 ± 0.9 91 47.1 ± 0.
C-10 CLINICAL STUDY - DECREASE HF upper one-sided 95% confidence bound were less than zero. The observed upper one-sided confidence bound for LV Offset was -19.4 points. All patients with data at a minimum of one visit, N=205 20 QOL Score 30 40 50 60 Baseline 3-Month LV Offset Figure C-5. Table C-6. 6-Month BiV-CRT Improvement in Quality of Life at Six months Improvement in QOL at six months. Statistic LV Offset Na Baseline BiV-CRT Estimate ± SE Na Estimate ± SE 100 54.6 ± 1.4 98 54.
CLINICAL STUDY - DECREASE HF C-11 if the lower one-sided 95% confidence bound of the percentage of patients improving one or more NYHA Class were greater than zero. The observed lower one-sided confidence bound for LV Offset was 47.9%. All patients with data at a minimum of one visit, N=187 100 Percent of Patients Improved 80 60 40 20 0 LV Offset Figure C-6. Table C-7.
C-12 CLINICAL STUDY - DECREASE HF Table C-8. Six-month change in NYHA by treatment group (continued) 6-Month Change in NYHAa LV Offset (N=95) BiV-CRT (N=92) Total (N=187) 35 (36.8) 36 (39.1) 71 (38.0) 6 (6.3) 2 (2.2) 8 (4.3) No Change Worsened 1 Class a. All patients with paired data; N=187. Device Effectiveness Primary Endpoint Ventricular Tachycardia/Fibrillation Detection Time––The objective of this endpoint was to demonstrate that CRT does not affect the ability to detect VT/VF.
CLINICAL STUDY - DECREASE HF C-13 Table C-10 on page C-13 summarizes the heart failure related adverse event rates through the six-month visit. A Kaplan-Meier analysis is also presented in Figure C-7 on page C-14 to show time to events. Table C-10. Heart failure-related adverse event free rate at six months Adverse Eventa Number of Events Number of Patients Heart Failure Adverse Event Free Rate Lower One-Sided 95% Confidence Bound Multiple heart failure symptoms 38 29 91.4 88.
C-14 CLINICAL STUDY - DECREASE HF All patients implanted and active at the randomization follow-up; N=338. 100 Event-Free Rate Lower One-Sided 95% Confidence Bound Percent Free from HF AE 90 80 70 60 Acceptance Boundary 50 N 40 338 313 0 1 300 290 279 267 258 2 3 4 5 6 Months from Randomization Visit Figure C-7.
CLINICAL STUDY - DECREASE HF C-15 The null hypothesis was to be rejected if the lower one-sided 95% confidence bound for system related complication rate through six months post-implant were greater than 70%. The system related complication free rate at six months was 83.2% with a lower 95% confidence bound of 79.7%. All patients implanted or attempted; N=358.
C-16 CLINICAL STUDY - DECREASE HF The mean percentage of appropriately paced beats during activities of daily living was 99.5 ± 1.3 with a median of 100.0% (p <0.01) (Table C-12 on page C-16). Table C-12. Continuous appropriate pacing during activities of daily living Statistica Result N 69 99.5 ± 1.3 Mean ± SD Median 100.0 Range 93.1 - 100.0 P-valueb <0.01 a. All patients in the Holter Substudy; N=69. b. P-value calculated from a signed-rank test.
CLINICAL STUDY - DECREASE HF Table C-13. Continuous appropriate pacing during exercise (continued) Statistica Range Result 90.3 - 100.0 P-valueb < 0.01 a. All patients in the Holter Substudy; N=67. b. P-value calculated from a signed-rank test.
C-18 CLINICAL STUDY - DECREASE HF - DRAFT -
D-1 CLINICAL STUDY - CONTAK CD APPENDIX D CLINICAL STUDY POPULATIONS Guidant CRT-Ds, when compared to OPT alone, have been demonstrated with reasonable assurance, to be safe and effective in significantly reducing: the risk of a composite of all-cause mortality or first hospitalization by 20%, the risk of all-cause mortality by 36%, and heart failure symptoms in patients who have moderate to severe heart failure (NYHA III/IV) including left ventricular dysfunction (EF ≤ 35%) and QRS duration ≥120 ms and re
D-2 CLINICAL STUDY - CONTAK CD EASYTRAK lead. An additional 510 patients initially underwent an implant procedure to receive the Model 1823 CONTAK CD CRT-D along with the EASYTRAK (Models 4510/4511/4512/4513) coronary venous, single-electrode pace/sense lead for a total of 517 patients who underwent an EASYTRAK lead implant procedure. In 69 patients the EASYTRAK lead implant attempt was unsuccessful.
CLINICAL STUDY - CONTAK CD Table D-1. D-3 Adverse events through randomization period (continued) # Of Events (# of pts) % Complications (Patients) Complications per 100 Device Months (Events) % Observations (Patients) Observations per 100 Device Months (Events) Loss of capture 10 (9) 0.6 (3) 0.1 (3) 1.2 (6) 0.3 (7) Elevated DFTs 6 (6) 0.4 (2) 0.1 (2) 0.8 (4) 0.2 (4) Inappropriate shock above rate cutoff 49 (38) 0.4 (2) 0.1 (2) 7.2 (37) 1.
D-4 CLINICAL STUDY - CONTAK CD Table D-1. Adverse events through randomization period (continued) # Of Events (# of pts) % Complications (Patients) Complications per 100 Device Months (Events) % Observations (Patients) Observations per 100 Device Months (Events) Cardiovascular-Related Events AV Block 3 (3) 0.0 (0) 0.0 (0) 0.6 (3) 0.1 (3) Arrhythmia - SVT 49 (42) 0.2 (1) 0.0 (1) 7.9 (41) 1.8 (48) Arrhythmia - VT 20 (17) 1.0 (5) 0.2 (5) 2.7 (14) 0.
D-5 CLINICAL STUDY - CONTAK CD Table D-1. Adverse events through randomization period (continued) # Of Events (# of pts) % Complications (Patients) Complications per 100 Device Months (Events) % Observations (Patients) Observations per 100 Device Months (Events) Subtotal CardiovascularRelated Events 358 (200) 7.7 (40) 1.6 (42) 35.6 (184) 12.2 (316) Total NoncardiovascularRelated Events 142 (92) 6.2 (32) 1.5 (39) 13.5 (70) 4.0 (103) Deaths A total of 109 deaths occurred during the study.
D-6 CLINICAL STUDY - CONTAK CD or CRT On (VDD). The study began as a crossover design (called "Phase I") and enrolled 248 patients with a primary endpoint of functional status with three months of follow-up. The study was later modified to a parallel design (called "Phase II") and enrolled 333 patients with a longer, six-month follow-up. The data from the first three months of the crossover phase were pooled with data obtained from the six-month parallel phase.
CLINICAL STUDY - CONTAK CD D-7 • Require in-hospital continuous intravenous inotropes • Have pre-existing cardioversion/defibrillation leads other than those specified in this investigational plan (unless the investigator intends to replace them with permitted cardioversion/defibrillation leads) • Women who are pregnant or not using medically accepted birth control • Have a mechanical tricuspid prosthesis • Involved in other cardiovascular clinical investigations of active therapy or treatment F
D-8 CLINICAL STUDY - CONTAK CD DEMOGRAPHIC DATA The CONTAK CD Study included patients with symptomatic heart failure despite optimal drug therapy as defined in the inclusion criteria. The population included patients who were NYHA Class II, III, or IV at the time of implant.
CLINICAL STUDY - CONTAK CD • • Lead and System Effectiveness – Lead––left ventricular pacing thresholds, biventricular sensing, biventricular lead impedance, and lead placement success rate – System––VF detection time and biventricular ATP effectiveness Lead and System Safety – Lead––incidence of lead-related adverse events – System––incidence of severe, device-related adverse events and operative mortality STUDY RESULTS Patient Accountability (Figure D-1 on page D-10) - DRAFT - D-9
D-10 CLINICAL STUDY - CONTAK CD Enrolled n = 581 14 Withdrew prior to surgery (“Intent”) 66 Unable to implant lead (“Attempt”) Implanted n = 501 10 Death 1 Withdrew Randomized n = 490 Control (No CRT) n = 245 Three months n = 99 Figure D-1.
CLINICAL STUDY - CONTAK CD Table D-3. Pre-implant assessment All Patients Characteristic Age at Implant (years) Gender [N (%)] NYHA Class [N (%)] Concomitant Medications [N (%)] Qualifying LVEF (%) PR D-11 Intervalb (ms) Qualifying QRS Durationb (ms) Resting Heart Rate ( bpm) CRT (N = 248) No CRT (N = 253) 248 253 Mean ± SD 66.0 ± 10.5 66.3 ± 10.5 Range 26.1 - 82.6 29.5 - 86.3 Male 210 (84.7) 211 (83.4) Female 38 (15.3) 42 (16.6) II 80 (32.3) 83 (32.8) III 148 (59.
D-12 CLINICAL STUDY - CONTAK CD Table D-3. Pre-implant assessment (continued) All Patients Characteristic Systolic Blood Pressure (mmHg) Diastolic Blood Pressure (mmHg) NYHA Class III/IV CRT (N = 248) No CRT (N = 253) P-valuea CRT (N = 117) No CRT (N = 110) P-valuea Mean ± SD 73 ± 12 75 ± 14 0.37 75 ± 13 74 ± 15 0.
CLINICAL STUDY - CONTAK CD Table D-4. D-13 Pre-implant history (continued) All Patients Characteristic CRT (N = 248) No CRT (N = 253) P-valuea CRT (N = 117) No CRT (N = 110) P-valuea 133 (53.6) 138 (54.5) 0.83 59 (50.4) 59 (53.6) 0.55 RBBB 35 (14.1) 31 (12.3) 21 (17.9) 14 (12.7) Non-Specific 80 (32.3) 84 (33.2) 37 (31.6) 37 (33.6) 167 (67.3) 178 (70.4) 76 (65.0) 78 (70.9) 81 (32.7) 75 (29.6) 41 (35.0) 32 (29.
D-14 CLINICAL STUDY - CONTAK CD inTable D-6 on page D-14. The Kaplan-Meier curve, showing total survival by treatment group, is shown in Figure D-2 on page D-14. Table D-6. Mortality stratified by treatment group and cause Deathsa Patients with CRT (N = 245) Patients with No CRT (N = 245) Cardiac, pump failure 4 (1.6%) 9 (3.7%) Cardiac, arrhythmic 1 (0.4%) 0 (0.0%) Cardiac, other 2 (0.8%) 1 (0.4%) Noncardiac 2 (0.8%) 3 (1.2%) Unknown 2 (0.8%) 3 (1.2%) Total 11 (4.5%) 16 (6.5%) a.
CLINICAL STUDY - CONTAK CD Table D-7. D-15 Patients hospitalized during treatment period Reason for Hospitalizationa All Patients NYHA Class III/IV CRT (N = 245) No CRT (N = 245) Total (N = 490) CRT (N = 117) No CRT (N = 110) Total (N = 227) Heart failure 32 39 71 23 27 50 Cardiac, other 20 25 45 14 14 28 Noncardiac 26 19 45 14 14 28 Total Hospitalizations 66 70 136 40 46 86 a. All patients implanted and active at 31 days post-implant; N = 490.
D-16 CLINICAL STUDY - CONTAK CD Table D-8. Change in Peak VO2 (continued) All Patients Peak VO2 (ml/kg/min) NYHA Class III/IV CRT (N = 216) No CRT (N = 201) P-valuea CRT (N = 96) No CRT (N = 80) P-valuea 3 Months 14.3 ± 0.2 13.9 ± 0.2 0.206 12.8 ± 0.4 12.1 ± 0.4 0.084 6 Months 14.4 ± 0.3 13.6 ± 0.3 0.030 13.8 ± 0.5 12.0 ± 0.5 0.003 a. P-values reflect the between-group differences with respect to baseline.
CLINICAL STUDY - CONTAK CD Table D-9. D-17 Change in Six-Minute Walk (continued) All Patients Six Minute Walk Distance (meters) NYHA Class III/IV CRT (N = 224) No CRT (N = 200) P-valuea CRT (N = 99) No CRT (N = 90) P-valuea 3 Months 348 ± 7 331 ± 8 0.058 312 ± 12 280 ± 12 0.028 6 Months 353 ± 8 332 ± 8 0.043 327 ± 14 288 ± 15 0.029 a. P-values reflect the between-group differences with respect to baseline.
D-18 CLINICAL STUDY - CONTAK CD Table D-10. Change in Quality of Life (continued) All Patients QOL (points) NYHA Class III/IV CRT (N = 234) No CRT (N = 225) P-valuea CRT (N = 107) No CRT (N = 96) P-valuea 3 Months 36.6 ± 1.5 37.3 ± 1.6 0.711 41.9 ± 2.4 47.5 ± 2.6 0.078 6 Months 34.8 ± 1.8 36.9 ± 1.8 0.395 37.2 ±- 3.1 47.3 ± 3.2 0.017 a. P-values reflect the between-group differences with respect to baseline.
D-19 CLINICAL STUDY - CONTAK CD Table D-11. Change in NYHA Class (continued) All Patients Change in NYHA Class CRT (N = 109) No CRT (N = 116) N % N Worsen 1 Class 13 11.9 Worsen 2 or More Classes 1 0.9 NYHA Class III/IV P-valuea CRT (N = 45) No CRT (N = 48) % N % N % 19 16.4 2 4.4 4 8.3 1 0.9 0 0.0 0 0.0 P-valuea a. P-value was calculated from Mantel-Haenszel test and reflects the between-group differences with respect to baseline.
D-20 CLINICAL STUDY - CONTAK CD Table D-12. Echocardiography results (continued) Parameter LVEF (%) Timepoint CRT No CRT Between Groups N Mean ± SE N Mean ± SE Mean ± SE P-value Change at 6 Months 104 -5.4 ± 1.1 92 -0.6 ± 1.1 -4.8 ± 1.5 0.002 Post-recovery Visit 99 26.9 ± 0.5 91 26.9 ± 0.5 0 – – Change at 6 Months 99 6.0 ± 1.1 91 2.3 ± 1.2 3.7 ± 1.7 0.
D-21 CLINICAL STUDY - CONTAK CD shown in Figure D-7 on page D-21 and Table D-15 on page D-21 are well within this limit. LV Pacing Threshold (V at 0.5 ms) 6 Acceptance Boundary 4 90% Tolerance Interval 2 0 0 6 12 18 24 Implant Duration (months) Figure D-7. EASYTRAK lead threshold measurements Table D-15. EASYTRAK lead threshold measurements Statistica Implant 3 Months 6 Months 12 Months 18 Months 24 Months 435 347 330 233 103 25 Mean ± SD 1.8 ± 1.2 1.7 ± 1.3 1.9 ± 1.5 1.
D-22 CLINICAL STUDY - CONTAK CD BiV R-wave Amplitude (mV) 15 Mean 10 5 Acceptance Boundary 0 0 6 12 18 24 Implant Duration (months) Figure D-8. EASYTRAK biventricular-sensed R-wave amplitude Table D-16. EASYTRAK biventricular-sensed R-wave amplitude Statistica Implant 3 Months 6 Months 12 Months 18 Months 24 Months 433 346 326 220 99 23 Mean ± SD 10.0 ± 5.2 9.9 ± 4.4 9.9 ± 4.5 9.8 ± 4.4 8.9 ± 3.5 8.5 ± 3.3 Upper Tolerance Limit 1.9 - 25.0 1.4 - 25.0 1.7 - 25.0 1.
D-23 CLINICAL STUDY - CONTAK CD BiV Lead Impedance (Ω) 400 Lower Bound of 95% CI 300 200 Acceptance Boundary 0 0 6 12 18 24 Implant Duration (months) Figure D-9. EASYTRAK biventricular pacing impedance Table D-17.
D-24 CLINICAL STUDY - CONTAK CD Table D-18. Reasons for unsuccessful EASYTRAK lead implant (continued) # of ptsa % Extracardiac stimulation 1 1.4 Inability to place an atrial pace/sense lead 1 1.4 Total 69 100 Reason a. Patients with unsuccessful attempt to implant EASYTRAK lead; N = 69. Table D-19.
CLINICAL STUDY - CONTAK CD D-25 Biventricular ATP Conversion Effectiveness Performance––the conversion rate of induced monomorphic ventricular tachycardia (MVT) was 64% and that of spontaneous MVT was 88%. Ventricular Tachyarrhythmia Detection Time––the VENTAK CHF and CONTAK CD devices sense events from both ventricles simultaneously. Ventricular tachyarrhythmia detection time was analyzed to determine if the additional lead had an adverse effect on sensing VT/VF.
D-26 CLINICAL STUDY - CONTAK CD rate was 14.5% (95% CI [11.5–17.5%]). Table D-21 on page D-26 reports lead-related adverse events observed during the CONTAK CD Study. Table D-21. EASYTRAK lead-related adverse events Adverse Eventsa Total % of pts (95% Cl) Lead-Related, N = 448 Loss of capture/lead dislodgment 31b 6.9 (4.6–9.3) Ventricular oversensing 11 2.5 (1.0–3.9) Extracardiac stimulation 9 2.0 (0.7–3.3) Insulation breach 2 0.4 (0.0–1.
CLINICAL STUDY - CONTAK CD • D-27 Transient renal failure (5 patients, 1.0%) These events were typically resolved without intervention and no permanent long-term sequelae were reported. Severe, Device-Related Adverse Events and Operative Mortality––the incidence of severe, device-related events was reported in 7 of 567 patients (1.2%); this was significantly less than the hypothesized rate of 20% (p < 0.01) (Table D-22 on page D-27).
D-28 CLINICAL STUDY - CONTAK CD Table D-24. Cause of death for operative mortality Implants N = 501 Attempts N = 66 Totala N = 567 Cardiac: pump failure 5 1 6 Cardiac: arrhythmic 2 1 3 Noncardiac 2 0 2 Unknown 1 0 1 Total 10 2 12 Cause of Death a. All patients attempted or implanted, N = 567.
CLINICAL STUDY - CONTAK CD D-29 Complication-free Rate (%) 90 85 80 75 Acceptance Boundary 70 0 Figure D-11. All Patients (NYHA Class II / III / IV) NYHA Class III / IV System safety Verification of CRT Delivery The delivery of biventricular pacing throughout the CONTAK CD Study was confirmed by comparing the programmed device output to the biventricular pacing threshold and demonstrating that capture was maintained in daily activities and during exercise.
D-30 CLINICAL STUDY - CONTAK CD FOCUSED CONFIRMATORY STUDY Study Design The Focused Confirmatory Study (FCS) was a prospective, multicenter study conducted in the United States in 127 patients who participated in an exercise performance study. The purpose of the FCS was to confirm effectiveness results related to functional capacity measures, specifically the Peak VO2 and 6-Minute Hall Walk, previously reported in the NYHA Class III/IV subgroup of the CONTAK CD Study.
CLINICAL STUDY - CONTAK CD Table D-26.
D-32 CLINICAL STUDY - CONTAK CD • Age ≥ 18 years • Optimal pharmacologic therapy for heart failure • Able to walk between 150 and 425 m in a Six-Minute Walk test Major Differences Between CONTAK CD and Focused Confirmatory Study Patients The CONTAK RENEWAL 3, CONTAK RENEWAL, and CONTAK CD devices provide the same cardiac resynchronization therapy (biventricular pacing) and have the same Indications for Use.
CLINICAL STUDY - CONTAK CD D-33 • Patients in the FCS had baseline measurements performed prior to implant. Patients in the CONTAK CD Study had baseline measurements performed post-implant, but before programming of the randomized therapy. • Seventy-seven percent of patients in the FCS (98 of N = 127) were on beta blockers compared to 42% in the CONTAK CD Study (95 of N = 227).
D-34 CLINICAL STUDY - CONTAK CD - DRAFT -
E-1 CLINICAL STUDY - CONTAK RENEWAL APPENDIX E CLINICAL STUDY POPULATIONS Guidant CRT-Ds, when compared to OPT alone, have been demonstrated with reasonable assurance, to be safe and effective in significantly reducing: the risk of a composite of all-cause mortality or first hospitalization by 20%, the risk of all-cause mortality by 36%, and heart failure symptoms in patients who have moderate to severe heart failure (NYHA III/IV) including left ventricular dysfunction (EF ≤ 35%) and QRS duration ≥120 ms a
E-2 CLINICAL STUDY - CONTAK RENEWAL • Able to understand the nature of the procedure • Available for follow-up on a regular basis at an approved investigational center Patients were excluded from the investigation if they met any of the following criteria: • Life expectancy of less than six months due to other medical conditions • For women: Pregnancy or absence of medically accepted birth control • Inability or refusal to sign the Patient Informed Consent • Inability or refusal to comply with
CLINICAL STUDY - CONTAK RENEWAL Table E-1. E-3 Pre-implant characteristics of study patient (continued) Characteristicsa Patient Data PR Interval 211 ± 49 ms Resting HR 70 ± 12 bpm a. Continuous measures are reported as means ± standard deviations. VENTRICULAR TACHYARRHYTHMIA DETECTION TIME The CONTAK RENEWAL device has independent Left Ventricular and Right Ventricular Sensing.
E-4 CLINICAL STUDY - CONTAK RENEWAL Inclusion/Exclusion Criteria Patients who were enrolled in the study were required to meet the following inclusion criteria: • Availability for 24 hours follow-up at an approved study center • Willingness and ability to participate in all testing associated with this study • Age 18 or above, or of legal age to give informed consent as specified by national law • Implanted with the CONTAK RENEWAL system for at least 1 month • Stable when programmed according to
CLINICAL STUDY - CONTAK RENEWAL Table E-2. E-5 Pre-implant characteristics of study patients (continued) Patient Data Characteristics IV 7 (15.2)% I 9 (19.6%) II 25 (54.3%) III 11 (23.9%) IV 1 (2.2%) Mean ± SD 8.3 ± 4.1 Range 1.5 – 15.0 Median 9.0 NYHA current [N (%)] Duration implanted (months) Programming Parameters Refer to the Pacing Therapies chapter for information about programming to maintain CRT.
E-6 CLINICAL STUDY - CONTAK RENEWAL Table E-3. Type of exercise testing performed (continued) Exercise Performed Number of Patients Stair Climbing 14 (30.4%) Total Table E-4. 46 Duration and intensity of exercise testing Results (N = 46) Borg RPE Rating Obtained Duration of Exercise (minutes) Maximum HR Obtained (bpm) 15 ± 1 Mean ± SD Median 15 Range 7 – 18 6.6 ± 3.3 Mean ± SD Median 6.
CLINICAL STUDY - CONTAK RENEWAL E-7 Pacing During Exercise The mean percentage of appropriately continuously paced beats during exercise was calculated as 98.3 ± 5.6% with a median of 100% and is summarized in Table E-6 on page E-7. Continuous appropriate BiV pacing is defined as pacing provided between the lower rate limit and the MTR, excluding PVCs. Table E-6. Exercise: continuous appropriate BiV pacing Statistic P-value Mean ± SD 98.3 ± 5.6 – Range 68.1 – 100 – Median 100 <0.
E-8 CLINICAL STUDY - CONTAK RENEWAL - DRAFT -
F-1 CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY APPENDIX F CLINICAL STUDY DESIGN NOTE: The SmartDelay optimization feature was previously known as Expert Ease for Heart Failure (EEHF+). This clinical investigation was a 50 patient, multi-center, acute hemodynamic study at 5 centers in the United States to validate the performance of Expert Ease for Heart Failure AV delay optimization algorithm (EEHF+1).
F-2 CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY • Patients in AF that can not be cardioverted for the study • Sustained, uncontrolled ventricular tachycardia • Frequent ectopic activity that makes stable hemodynamic measurements infeasible • Sinus rhythm < 30 bpm or > 100 bpm • Complete AV node block • Acute severe heart failure exacerbation • Severe aortic valvular stenosis (valve area < 1.
CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY Table F-1. F-3 Subject Demographics Characteristic Measurement Result Age at Implant Number of subjects 50 Mean ± SD 68.1 ± 10.5 Range [47.0, 85.0] Female 12 (24.0) Male 38 (76.0) II 1 (2.0) III 49 (98.0) Number of subjects 50 Mean ± SD 26.6 ± 6.6 Range [5.0, 35.0] LBBB 38 (86.4) RBBB 12 (27.
F-4 CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY Correlation between maximum achievable %LV dP/dtmax and the %LV dP/dtmax achieved with the EEHF+ delay for both atrial sensing (left, n=38) and atrial pacing (right, n=36). Figure F-1.
CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY F-5 Differences between %LV dP/dtmax achieved with EEHF+ and with fixed AV delays of 100 ms, 120 ms, 140 ms or 160 ms for atrial sensing (left) and atrial pacing (right). A negative value indicates that the EEHF+ algorithm is better. The box represents the mean and error bars represent 95% CI of mean. Figure F-2. Differences, achieved with EEHF+ and fixed AV delays Table F-2.
F-6 CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY Table F-2. Differences between maximal achievable %LV dP/dt max and that achieved using EEHF+ and a fixed AV delay of 100 ms, 120 ms, 140 ms and 160 ms, during atrial sensing (continued) n, mean ± std, 95% CI n, mean ± std, 95% CI n, mean ± std, 95% CI Paired t-test EEHF+ 160 ms Paired difference P-value 33, -1.1 ± 1.3, (-1.6, -0.7) 33, -3.6 ± 3.8, (-4.9, -2.3) 33, -2.5 ± 4.0, (-3.8, -1.1) 0.0013 Table F-3.
CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY F-7 Differences between %LV dP/dtmax achieved with EEHF+ and with two echo-based methods: the Ritter method and the AoVTI method for atrial sensing (left) and atrial pacing (right). A negative value indicates that EEHF+ was better. The box represents the mean and error bars represent 95% CI of mean. Figure F-3. Differences, achieved with EEHF+ and echo-based methods Table F-4.
F-8 CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY Table F-5. Differences between maximal achievable %LV dP/dt max and that achieved from the EEHF+, the Ritter method, and the AoVTI method during atrial pacing (continued) n, mean ± std, 95% CI n, mean ± std, 95% CI n, mean ± std, 95% CI Paired t-test EEHF+ AoVTI method Paired difference P-value 34, -2.0 ± 2.6, (-2.8, -1.1) 34, -2.8 ± 2.9, (-3.8, -1.8) 34, -0.9 ± 2.6, (-1.8, 0.0) 0.
CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY F-9 Table F-6. Differences between maximal achievable %AoVTI and that achieved using the EEHF+ and a fixed AV delay of 100 ms, 120 ms, 140 ms, and 160 ms during atrial sensing. (continued) n, mean ± std, 95% CI n, mean ± std, 95% CI n, mean ± std, 95% CI Paired t-test EEHF+ 160 ms Paired difference P-value 36, -8.5 ± 8.3, (-11.2, -5.8) 36, -7.3 ± 6.4, (-9.4, -5.2) 36, 1.2 ± 9.8, (-2.0, 4.4) 0.4769 Table F-7.
F-10 CLINICAL STUDY - SUMMARY OF CRT OPTIMIZATION ALGORITHM VALIDATION STUDY Table F-8. Differences between maximum achievable %AoVTI and that achieved with EEHF+ and Ritter during atrial sensing n, mean ± std, 95% CI n, mean ± std, 95% CI n, mean ± std, 95% CI Paired t-test EEHF+ Ritter method Paired difference P-value 36, -8.5 ± 8.3, (-11.2, -5.8) 36, -6.5 ± 5.6, (-8.3, -4.6) 36, 2.0 ± 9.1, (-0.9, -5.0) 0.1895 Table F-9.
G-1 CLINICAL STUDY - VITALITY APPENDIX G CLINICAL STUDY POPULATIONS Guidant CRT-Ds, when compared to OPT alone, have been demonstrated with reasonable assurance, to be safe and effective in significantly reducing: the risk of a composite of all-cause mortality or first hospitalization by 20%, the risk of all-cause mortality by 36%, and heart failure symptoms in patients who have moderate to severe heart failure (NYHA III/IV) including left ventricular dysfunction (EF ≤ 35%) and QRS duration ≥120 ms and rem
G-2 CLINICAL STUDY - VITALITY Results A total of 100 patients were enrolled in this study. Of these, 96 patients were successfully implanted, with 4 intents. Ninety-three (93) patients finished their 1-month follow-up per the study protocol. All primary and secondary endpoints of this study were met. The results from this study provide evidence of the safety and effectiveness of the VITALITY with Automatic Intrinsic Rhythm ID algorithm (Table G-1 on page G-2). Table G-1.
CLINICAL STUDY - VITALITY Table G-1. G-3 VITALITY Chronic Study Results (continued) Automatic Rhythm ID Accuracy (1 month) 97.7% Manual Rhythm ID Accuracy (1 month) 100% a. GEE adjusted specificity = 93.7% b. Combined specificity includes both Induced and Spontaneous data.
G-4 CLINICAL STUDY - VITALITY The VT/VF detection time of the VITALITY ICD was found to be within two seconds of the VENTAK PRIZM 2 detection time, leading to the conclusion that activating the additional VITALITY features does not have a negative effect on the existing ICD sensing and detection functionality (Table G-2 on page G-4). Table G-2. Acute study results Study Endpoint VT/VF Detection Time (seconds) VITALITY (Mean ± std) N VENTAK PRIZM 2 DR (Mean ± std) N 3.60 ± 0.60 N = 47 3.52 ± .
H-1 CLINICAL STUDY - SUMMARY OF GDT1000 SENSING ACUTE STUDY APPENDIX H CLINICAL STUDY POPULATIONS GDT1000 study included patients indicated for a CRT-D device.
H-2 CLINICAL STUDY - SUMMARY OF GDT1000 SENSING ACUTE STUDY Protocol Testing Four scenarios were tested, including different combinations of sensed atrial signals (AS), paced atrial signals (AP), sensed ventricular signals (VS), and paced ventricular signals (VP), i.e., AS/VS, AS/VP, AP/VS, and AP/VP. Sensing algorithm performance was analyzed from patients’ real-time electrograms (EGM) and electronic signals.
CLINICAL STUDY - SUMMARY OF GDT1000 SENSING ACUTE STUDY H-3 STUDY RESULTS Patient Characteristics The table below shows the characteristics of the patients implanted or attempted (Table H-1 on page H-3). Table H-1. All patients implanted or attempted, Phase 1 and Phase 2 Characteristic Measurement Phase 1 Result (N=29) Phase 2 Result (N=19) Age at implant Mean ± SD 65.8 ± 12.2 68.1 ± 9.6 Range [44.6, 85.5] [51.3, 81.8] Gender [N (%)] Female 14 (48.0) 14 (74.0) Male 15 (52.0) 5 (26.
H-4 CLINICAL STUDY - SUMMARY OF GDT1000 SENSING ACUTE STUDY placed in the septal wall (0/1) and unspecified location (1/0). A majority of the left ventricular leads were implanted in the lateral, postero-lateral, or posterior wall (21/15), with the remaining placed in an antero-lateral, anterior, or postero-septal location (4/3). Lead Configurations In this study, both RA and RV leads used a bipolar configuration, which was not programmable.
CLINICAL STUDY - SUMMARY OF GDT1000 SENSING ACUTE STUDY H-5 sensed events (223 undersense and 833 oversense events). The sensing algorithm used in the first phase achieved the sensitivities, specificities, positive predictive values (PPV), rates of undersensing (1-sensitivity), and rates of oversensing (1-PPV) are summarized in the table below (Table H-3 on page H-5). Table H-3.
H-6 CLINICAL STUDY - SUMMARY OF GDT1000 SENSING ACUTE STUDY Table H-4. Left Ventricular Channel Summary of Sensing Performance - Second Phase (continued) Specificity Sensitivity (Rate of Undersensing) Positive Predictive Value (Rate of Oversensing) Appropriate Sensed Beats Inappropriate Sensed Beats: Undersense Inappropriate Sensed Beats: Oversense 99.98% (0.016%) 99.99% (0.008%) 12,227 2 1 35,831 2 169 99.
CLINICAL STUDY - SUMMARY OF GDT1000 SENSING ACUTE STUDY H-7 Undersense Events LV undersense events (223) in the first phase of the study primarily occurred in one patient whose LV intrinsic amplitude was less than 1.0 mV, which is much smaller than the clinically acceptable threshold. This small LV intrinsic amplitude resulted in undersensing some LV events. Two LV undersense events occurred in the second phase of the study.
H-8 CLINICAL STUDY - SUMMARY OF GDT1000 SENSING ACUTE STUDY - DRAFT -
INDEX Symbols 50 Hz/manual burst pacing 8-9 A A-blank after RV-sense 5-57 after V-pace 5-57 A-tachy response (ATR) mode switch 5-27 ABM (Autonomic Balance Monitor) 7-4 Accelerate, in zone 4-3 Accelerometer 5-21 activity threshold 5-22 reaction time 5-23 recovery time 5-26 response factor 5-24 Activity threshold 5-22 Adaptive-rate pacing 5-20 Adverse event 1-19 AFib rate threshold 3-29, 3-36, 3-38 Amplitude 5-16 ATP (antitachycardia pacing) 4-18 intrinsic test 6-7 Application screen 2-5 Arrhythmia logbook 7
B Backup VVI pacing during atrial stimulation, EP test 8-2 Battery Beginning of life (BOL) 6-2 Explant status 6-2 icon 2-9 indicator 6-2 status 6-2 Beep during capacitor charge 6-5 feature setup 10-4 Biventricular trigger 5-33 maximum pacing rate 5-34 Blanking A-blank after RV-sense 5-57 A-blank after V-pace 5-57 Blanking; Noise rejection, blanking 5-56 Burst ATP (antitachycardia pacing) 4-11 cycle length (BCL) 4-14 minimum interval 4-14 number of bursts 4-11 pacing, 50 Hz/manual burst 8-9 parameter 4-11 pu
onset 3-34 rate sensing 3-3 rate threshold 3-4 reconfirmation/committed shock 4-23 redetection 3-11 stability 3-32 sustained rate duration (SRD) 3-35 tachyarrhythmia 3-1 tachyarrhythmia, safety mode 2-19 V rate > A rate 3-28 vector timing and correlation 3-27 ventricular, initial 3-6 window 3-13 Device characteristics as shipped 1-23 description 1-4 mode 3-2 programming recommendation 5-2 specification 1-21 storage 1-8 Diagnostic battery status 6-2 heart rate variability (HRV) 7-12 histogram 7-11 lead test
F Fallback, atrial mode switch LRL 5-31 mode 5-30 time 5-31 Federal Communications Commission (FCC) 1-25 Fibrillation VFib induction 8-5 Follow-up examination, routine 10-2 predischarge 10-2 test 10-2 H Heart failure 5-2 Heart rate variability (HRV) 7-12 Histogram 7-11 Horizontal slider icon 2-9 I Icon battery 2-9 check 2-9 details 2-8 event 2-9 horizontal slider 2-9 increment and decrement 2-9 lead 2-8 patient 2-8 patient information 2-11 Programmer/recorder/monitor (PRM) mode indicator 2-6 run 2-9 scrol
intrinsic amplitude 6-7 pace threshold 6-8 test 6-6 Left ventricular protection period (LVPP) 5-55 Left ventricular refractory period (LVRP) 5-55 Logbook 7-5 Longevity pulse generator 1-26 Lower rate limit (LRL) 5-10 LV offset 5-14 LV-blank after A-pace 5-57 fallback ATR (atrial tachy response) 5-30 pacing 5-7 Programmer/recorder/monitor (PRM) 2-6 temporary, EP test 8-2 ventricular tachy 3-2 MTR (maximum tracking rate) 5-4 N Noise response 5-60 Nominal parameter setting A-1 Number of bursts 4-11 pulse cou
chamber, ventricular 5-14 lower rate limit (LRL) 5-10 LV offset 5-14 maximum sensor rate (MSR) 5-13 maximum tracking rate (MTR) 5-11 mode 5-7 noise response 5-60 Parameter, BASIC 5-7 post therapy 5-17, 5-18 post-therapy 5-17 programming recommendation 5-2 pulse width 5-15 refractory 5-52 runaway protection 5-11 sensitivity 5-16 sensor 5-19 SmartDelay optimization 5-50 temporary 5-18 therapy 5-6 Package content 1-22 symbol on 1-22 Parameter, characteristics 1-23 Patient counseling information 1-28 handbook 1
Quit Ending a telemetry session 2-14 R Radio frequency (RF) ending telemetry 2-14 interference 2-15 operating temperature, telemetry 2-14 starting telemetry 2-13 telemetry 2-12 Ramp scheme 4-15 Ramp/Scan scheme 4-17 Rate adaptive 5-20 AFib threshold 3-29 calculation 3-4 lower limit (LRL) 5-10 maximum sensor 5-13 maximum tracking 5-11 sensing 3-3 sustained rate duration (SRD) 3-35 threshold, ventricular 3-4 V rate > A rate 3-28 ventricular 3-4 zone 3-4 Rate enhancement, pacing 5-35 rate hysteresis 5-36 rate
Sensitivity adjustment 10-3 Sensor and trending, pacing 5-19 accelerometer 5-21 adaptive-rate 5-20 maximum sensor rate (MSR) 5-13 SmartDelay optimization 5-50 Setscrew locations 9-6 Setting parameter value A-1 zone configuration 3-4 Shock charge time, energy 4-22, 6-5 commanded, EP test 8-10 committed 4-23 diverting 2-16 energy 4-21 impedance 6-8 last delivered 6-6 on T induction 8-6 polarity 4-22 post-shock pacing 5-17, 5-18 redetection 3-18 selection 4-3 sequence 4-2 STAT SHOCK 2-17 therapy 4-21 ventricul
tachyarrhythmia 4-2 tachyarrhythmia, safety mode 2-19 Therapy history 7-2 arrhythmia logbook 7-5 counter 7-15 heart rate variability (HRV) 7-12 histogram 7-11 patient triggered monitor 7-17 Threshold AFib rate 3-29 rate 3-4 Threshold, activity 5-22 Time-out, ATP 4-18 Timing blanking 5-56 left ventricular protection period (LVPP) 5-55 PVARP after PVC 5-54 Timing, pacing 5-52 Toolbar 2-7 Tracking preference 5-36 Trending sensor 5-19 Trends 7-3 V V rate > A rate 3-28 Vector timing and correlation 3-27, 3-36 V
radio frequency (RF) 2-13 security 2-14 session 2-13, 2-14 Zone cardiac resynchronization therapy (CRT) delivery 3-5 configuration 3-4 ventricular 3-4 ventricular tachyarrhythmia 3-4 ZOOM LATITUDE Programming System components 2-2 ZOOMVIEW Software Application 2-2 purpose 2-2 screens and icons 2-5 use of color 2-10 - DRAFT -
- DRAFT -
Boston Scientific 4100 Hamline Avenue North St. Paul, MN 55112–5798 USA www.bostonscientific.com 1.800.CARDIAC (227.3422) +1.651.582.4000 © 2007 Boston Scientific or its affiliates All rights reserved.